what type of brain scan is needed to identify ocd
Introduction
Obsessive-compulsive disorder (OCD) is a neuropsychiatric disease characterized past obsessions and/or compulsions. Obsessions are recurrent, persistent, and unwanted thoughts, urges, or images that generate feet and/or distress that are alleviated transiently past compulsions, i.east., repetitive and ritualized behaviors (such as checking, washing, and ordering) or mental acts (such every bit counting, praying, or repeating words silently; American Psychiatric Association, 2013). Current first-line treatments for OCD include exposure and response prevention (ERP) and serotonin reuptake inhibitors (SRIs; Sookman and Fineberg, 2015). However, as non all patients respond satisfactorily to these treatments, other augmenting drugs (such as glutamate-modulating agents, amidst others) may need to be added to SRIs (Fineberg et al., 2006; Simpson et al., 2013; Modarresi et al., 2018). Clearly, to develop more effective treatments for OCD, a greater agreement of its etiology and pathophysiology is required.
Although the etiology of OCD remains unclear, research has revealed changes in the cortico-striatal-thalamic-cortical (CSTC) circuits of OCD patients (Pittenger et al., 2011). These circuits link areas that take of import roles in the executive function and regulation of behavior (Saxena et al., 2001) and may be well implicated in the mediation of OCD symptoms (Chamberlain et al., 2005). They include cortical and subcortical regions and the white thing (WM) tracts that link them. The cingulate parcel (CB), for instance, interconnects the cingulate cortex with limbic regions such equally the prefrontal cortex, striatum, and thalamus, and has already been implicated in other neuropsychiatric disorders (Sun et al., 2003; Catheline et al., 2010). The importance of the cingulum in OCD has been highlighted by its use as a target of deep encephalon stimulation and ablative procedures of treatment refractory OCD patients (Rauch, 2003).
Diffusion tensor imaging (DTI) is a method that allows the measurement of the diffusion characteristics of h2o molecules in vivo. This approach is widely used to investigate WM integrity in psychiatric disorders (Thomason and Thompson, 2011). Although decreased fractional anisotropy (FA) seems disseminated to several brain regions of individuals with OCD, such as the corpus callosum, the longitudinal superior and inferior fasciculus, and the inductive limb of the internal sheathing (Szeszko et al., 2005; Bora et al., 2011; Nakamae et al., 2011; Admon et al., 2012), the existing DTI literature suggests the CB to be one of the tracts nearly consistently affected by decreased WM integrity in developed samples (Piras et al., 2013; Koch et al., 2014). For instance, a recent systematic review found abnormalities in the cingulum in 10 out of the 17 studies (Piras et al., 2013), mostly decreased FA or increased hateful diffusivity (MD; consequent with decreased WM integrity; Garibotto et al., 2010; Nakamae et al., 2011). Another proxy for decreased WM integrity was also found in the corticospinal tract, internal capsule, and superior longitudinal fasciculus (Fontenelle et al., 2011).
Glutamate is the primary excitatory neurotransmitter in the encephalon and a primary neurotransmitter in CSTC circuitry (Shepherd, 2004). Information technology is synthesized from glutamine supplied by astrocytes (Ramadan et al., 2013). One time glutamate is released into the synaptic fissure, it is re-uptaken by astrocytes and converted into glutamine, which volition again be used as a precursor of glutamate (Ramadan et al., 2013). Studies using dissimilar methods propose that OCD patients might have a dysfunctional glutamatergic neurotransmission (Carlsson, 2001; Pittenger et al., 2006; Ting and Feng, 2008). For example, genetic association studies have reported that specific SNPs in or nearly gene SLC1A1 (which codes for a neural glutamate transporter) such equally rs301443, rs10491734, and rs7856675 are associated with OCD (Shugart et al., 2009; Samuels et al., 2011). GRIN2B, a gene that codes for a subunit of N-methyl-D-aspartate (NMDA) receptors, has also been associated with OCD (Arnold et al., 2009; Kohlrausch et al., 2016). Two studies establish elevated cerebrospinal fluid glutamate levels in OCD patients compared to controls (Chakrabarty et al., 2005; Bhattacharyya et al., 2009). There is now evidence of the efficacy of glutamatergic drugs in OCD (Grados et al., 2013; Rodriguez et al., 2013; Marinova et al., 2017). Finally, mice with knocked OUT glutamatergic genes nowadays OCD-like (preparation) beliefs (Pittenger et al., 2011).
Perhaps one of the virtually disseminated methods to assess glutamate and other metabolite levels in the encephalon is the proton magnetic resonance spectroscopy (H1-MRS). H1-MRS is a noninvasive method that permits in vivo quantification of brain biochemistry and has been applied to investigate glutamate levels on OCD. The molecular structures of glutamate and glutamine, which are very similar, give rise to similar magnetic resonance spectra (Ramadan et al., 2013). Equally a result, the combined glutamate and glutamine (Glx) levels are measured past the H1-MRS. The reports, however, have shown some apparent contradictory results. Studies have demonstrated that unmedicated children with OCD had increased Glx levels in the left caudate nucleus that declined after paroxetine treatment as compared to controls (Rosenberg et al., 2000). In adults, a reduction in the inductive cingulate cortex (ACC) Glx levels was restricted to women and negatively correlated with the severity of OCD symptoms (Yücel et al., 2008). Here, we used a multi-method approach combining H1-MRS and DTI techniques to investigate both the metabolic and the microstructural WM changes in OCD patients as compared to salubrious controls.
It is important to investigate the relationships betwixt WM integrity and H1-MRS parameters [eastward.one thousand., glutamate and N-acetylaspartate (NAA)] across different neuropsychiatric disorders. For instance, oligodendrocytes (glial cells largely responsible for WM synthesis) seem vulnerable to glutamate receptor-mediated excitotoxicity (McDonald et al., 1998). At that place is evidence suggesting that changes in NAA may reflect disturbed myelin synthesis (Chakraborty et al., 2001; Madhavarao et al., 2005; Wang et al., 2009; Arun et al., 2010). In salubrious adults, WM NAA explained a pregnant proportion of variability in the FA values, particularly in the splenium of corpus callosum (Wijtenburg et al., 2013). Although a handful of studies take attempted to correlate WM integrity to H1-MRS profile in schizophrenia (Steel et al., 2001; Tang et al., 2007; Rowland et al., 2009; Chiappelli et al., 2015; Reid et al., 2016), the human relationship between WM integrity and encephalon biochemistry in OCD patients remains understudied (Wang et al., 2017, 2018). In the first combined DTI-MRS study, Wang et al. found a positive correlation between FA in the dorsal ACC and choline. In the second, they investigated the anterior thalamic radiation and found a negative correlation between the mean fiber length in the right and ipsilateral thalamic choline level in patients. So far, the clan between structural abnormality in the CB and ACC metabolic contour has not been explored. Given the literature reviewed above, we hypothesized: (i) that OCD patients would exhibit decreased FA values in the CB and increased Glx levels in the ACC; (ii) that these findings would correlate with OCD symptomatology; (three) that they would exist independent from medication status; and (4) that the Glx levels in ACC will negatively correlate with FA in CB.
Materials and Methods
Participants
Patients with OCD who were under treatment in the Obsessive, Compulsive, and Anxiety Enquiry Program of the Federal University of Rio de Janeiro and age- and sex-matched healthy community controls participated in the study. All patients met clinical criteria for OCD according to the Diagnostic and Statistical Manual of Mental Disorders (DSM-4-TR), had their diagnosis confirmed using the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders (Del-Ben et al., 2001), and had total Yale–Brown Obsessive–Compulsive Scale (YBOCS; Goodman et al., 1989) scores ≥16. OCD patients and controls with mental retardation, previous suicidal attempts, psychotic disorders, antisocial personality, or contraindications to MRI were excluded from the report. Also, controls with history of obsessions and compulsions were excluded. All participants were older than 18 years and provided their written informed consent to participate in the enquiry protocol, which was canonical by the D'Or Institute for Research and Education review lath.
Clinical Assessments
All participants with OCD were interviewed using the YBOCS to evaluate the severity of OCD symptoms. They were also assessed for age at onset (and consequently duration of illness), severity of depression [with the Beck Depression Inventory (BDI; Cunha, 2001)], and functioning [with the Global Assessment of Operation (GAF)]. All patients were undergoing pharmacological treatment.
To rate the relative dose of antipsychotic and SRI or other antidepressants being used, scores were attributed to the therapeutically equivalent doses across different medications. According to this scoring system, a score of 1 corresponded to the minimally effective dose for a given SRI, which is likewise known to occupy at least 80% of the brain serotonin transporters in the striatum (Meyer et al., 2004). Therefore, we feel that the adopted strategy was clinically and biologically valid. Eventually, each participant received an SRI equivalent score, i.due east., zero to patients without medication; i to patients who were taking 20 mg of fluoxetine, paroxetine, or citalopram, 50 mg of sertraline, 100 mg of fluvoxamine, or 75 mg of clomipramine; ii to patients taking twice the minimally constructive doses; and so on and so forth. The score for relative dose of antipsychotic was based on doses equivalent to 100 mg of chlorpromazine (i.e., one for patients taking two mg of haloperidol, two mg of trifluoperazine, 2 mg of pimozide, 2 mg of risperidone, 5 mg of olanzapine, 7.v mg of aripiprazole, 75 mg of quetiapine, 100 mg of sulpiride, and 1,000 mg of thioridazine, and then on; Woods, 2003).
Imaging Acquisition
Anatomical images were obtained with an Achieva 3T scanner (Philips Medical Systems, Netherlands), using the following pulse sequences: 3D T1-weighted field repeat [repetition fourth dimension (TR)/echo time (TE)/matrix/field of view (FOV) = 7.ii ms/3.4 ms/240 × 240/240 mm, 170 slices, thickness sixty mm] and fluid attenuate inversion recovery [FLAIR; TR/TE/inversion fourth dimension (TI)/matrix/FOV = 11,000 ms/125 ms/two,800 ms/288 × 168/230 mm, 26 slices, gap = 1 mm, thickness = 4.5 mm]. Diffusion-weighted images (DWIs) were acquired in axial aeroplane with a unmarried-shot, spin-echo echoplanar sequences: TR/3TE/matrix/FOV = 5,582 ms/65 ms/96 × 95/240 × 240 (mm), slice thickness = 2.5 mm, 60 slices without gap. Diffusion sensitization gradients were practical in 32 non-collinear directions, with a b gene of ane,000 due south/mm2. H1-MRS findings were recorded using a point resolved spectroscopy volume selection (PRESS; TE 31 ms/TR 2,000 ms/2,048 points/2 kHz bandwidth). Voxel size was 30 × xxx × 15 mm and placed on the ACC bilaterally (Figure 1). Levels of total N-acetyl-aspartate (NAAt), glutamate and glutamine (Glx), choline (Cho), and creatine + phosphocreatine (Cr) were measured.
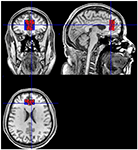
Figure 1. Example of the anatomical reference for the position of the volume of interest (VOI). Sagittal, coronal, and axial views.
Improvidence Tensor Imaging Procedures
Prior to analysis, participants' datasets received a numeric code and were divided into controls or OCD patients. All improvidence images were visually inspected for artifacts. Motion artifacts and eddy current distortion effects were corrected. Exclusion criteria included excessive movements and brain lesions. The DTI parameters used to investigate the WM integrity include FA and Md, the frequently used parameters, as they measure the directionality of water diffusion and the magnitude of diffusion, respectively. The diffusion tensor for each voxel was calculated based on the eigenvectors (v1, v2, v3) and eigenvalues (λ1, λ2, λ3). After the FA and MD maps were calculated from the eigenvalues, color-coded maps were generated from the FA values and 3 vector elements of v1 to visualize the WM tract orientation were performed (DTIFit 2.0, FDT-FMRIB'south Diffusion Toolbox, FSL). FA and Medico were brain-extracted (BET, DTIFit toolbox, office of FSL v.0.6, FMRIB software; Smith, 2002) and registered to a mutual space (Montreal Neurological Establish Template or MNI152) using constrained nonlinear registration (Image Registration Toolkit; Rueckert et al., 1999). The derived FA and Physician data were further analyzed using voxelwise whole-brain Tract based Spatial Statistics (TBSS 1.2, FSL; Smith et al., 2006; Simonyan et al., 2008) and Region of involvement (ROI) approaches to explore the WM integrity and differences amid groups. ROI analyses were selected according to their human relationship with OCD pathology and related anatomical changes previously reported.
Whole-Brain Analysis
Whole-brain voxelwise statistical analysis of FA and Medico were performed using TBSS in order to assess the differences in the WM fiber tracts between OCD patients and good for you volunteers. To preserve the intactness of WM construction, a voxelwise-specific tuned nonlinear registration method was used to annals FA and MD images into a standard infinite (Epitome Registration Toolkit; Rueckert et al., 1999). Aligned FA images were averaged to create the mean FA from all subjects. The mean FA was used to generate the hateful FA "skeleton tract," which represents the tracts shared by all subjects (Smith et al., 2006). Registered FA data from each subject were "projected" onto the hateful FA skeleton mask to generate the final skeletonized FA data.
A threshold was applied (FA >0.two) to restrict the statistical assay only to WM voxels that were successfully aligned across subjects, maintaining just the subject's major tract structures. To test for significant local FA and MD differences between controls and OCD, voxelwise cross-discipline statistical analysis was carried out using permutation-based not-parametric inference with 10,000 random permutations (FSL Randomize tool) on each voxel of the resulting "mean skeletonized" data (Rueckert et al., 1999) generating the statistical maps The statistical map was "thickened" using spatial smoothing in club to improve visualization.
ROI Analysis
ROIs were placed using a DTI–MRI atlas of human WM from Johns Hopkins University (JHU ICBM-DTI-81 White-Matter Labels and JHU WM Tractography Atlas) in the left and correct CB. The ROIs were automatically loaded onto the FA and Md maps and visually checked to ostend their location. FA and MD values were automatically extracted using FSL 5.0.half dozen, FMRIB software. Statistical analysis was performed with p < 0.05. Analyses including BDI scores and treatment scores as covariates were carried out to investigate associations between the FA and Md values and OCD severity assessed by Y-BOCS scores.
H1-MRS Procedures
Single-voxel H1-MRS was performed bilaterally and exclusively at the rostral ACC (30 × 30 × xv mmthree stock-still). The book of interest (VOI) was positioned to avoid the skullcap. The anatomical reference for the position of the VOI was the rostrum of the corpus callosum, angulated co-ordinate to its genu. T2-weighted scans and FLAIR were used to help the placement. Full H1-MRS examination time was approximately 4 min. Eddy electric current correction was performed for each discipline. LCModel (version six.3- 1H; Provencher, 1993) was used for spectrum quantification. An example of a spectrum is in the Supplementary Material. The amplitude (i.eastward., the surface area under the spectra) was firstly fitted for the major metabolites, including NAA, Glx, Cr, and Cho. To minimize changes in magnetic field homogeneity, nosotros used Cr signals as the reference, with the results presented as metabolite-to-Cr ratio, because Cr is relatively stable amongst other metabolites (Govindaraju et al., 2000). Results are presented in arbitrary units (a.u.). The H1-MRS parameters used for the present study provided robust signals for both the healthy controls and OCD groups in the ACC. The output from LCModel includes the signal-to-racket ratio (SNR) and the hateful Cramer–Rao lower spring (CRLB), which is a measure of reliability of the fit. We included participants who had CRLB (SD%) <20% and SNR ≥10. Specifically, healthy controls had an ACC SNR of 21.24 (SD v.09) and a total width at half maximum pinnacle top (FWHM) of 0.06 ppm (SD 0.02). OCD patients had an SNR of twenty.96 (SD 4.89) and an FWHM of 0.05 ppm (SD 0.02). None of these measures were different between the two groups (p = 0.86 and 0.26), suggesting that the quality of the data is comparable across the two groups. The CRLB for NAAt, Cr, Cho, and Glx were 5.one%, three.9%, 4.4%, and nine.5% (SD 2.71, 2.28, 1.89, and 2.73), respectively, for salubrious controls, and 4.3%, three.1%, 3.8%, and 8.iii% (SD two.42, 1.94, ane.69, and two.29), respectively, for patients.
Statistics
The t-exam was used to compare the means of age, schooling, GAF, and BDI amidst patients and controls. Metabolites were analyzed individually using the SPSS (5.twenty.0 IBM, Windows). To clarify the associations betwixt H1-MRS metabolite levels and continuous variables (such equally the YBOCS, BDI, and GAF scores), Spearman's correlation coefficients were performed. For FA and Md data candy using the FSL tool, statistical analyses of the voxelwise type of the whole encephalon were fabricated using non-parametric inference based on permutations, with ten,000 random permutations through the FSL randomization tool, in each voxel contained in the map FA and MD skeletonized mean. Results with a p-value of less than 0.05 were considered statistically significant, using family-wise error rate (FWE)-based TFCE (threshold-free cluster enhancement). The r values for FA and MD analysis were obtained from r = t/sqrt(t 2 + df). t-values were extracted using randomize (TBSS).
Results
Clinical Cess
A total of 23 OCD patients and 21 healthy volunteers participated in the report. The comparisons between age, sex activity, years of study, and GAF and BDI scores exhibited by OCD patients and good for you volunteers are shown in Tabular array one. There was no statistically significant divergence between OCD patients and the control group in terms of gender (p = 0.239), age (p = 0.561), and years of educational activity (p = 0.367; Table 1). However, compared to controls, OCD patients scored higher in the BDI (p ≤ 0.001) and lower in the GAF (p ≤ 0.001). Also, all patients were receiving medication for OCD, including clomipramine (n = 10), fluoxetine (due north = 8), sertraline (n = iv); paroxetine (n = 3), escitalopram (n = 2), and fluvoxamine (northward = 2). An additional 13 patients were receiving concomitant antipsychotics, vii beingness typical and half-dozen atypical. The mean Y-BOCS scores were 13.78 (3.0) for obsessions, xiii.91 (3.1) for compulsions, and 27.70 (5.seven) for both symptoms (full score). The hateful affliction duration was 25.17 (fifteen.9) years.
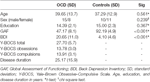
Table one. Comparing between some sociodemographic and clinical features of obsessive-compulsive disorder (OCD) patients vs. healthy controls.
H1-MRS Findings
In the ACC, NAAt/Cr levels did not significantly differ by group (p = 0.191). There were also no significant grouping differences in Cho/Cr levels (p = 0.454). However, compared with controls, OCD patients had significantly higher levels of Glx/Cr in the ACC (p = 0.016; Tabular array 2, Figure two).

Table 2. Comparison between metabolites' concentration in OCD vs. healthy controls in inductive cingulate cortex (ACC).
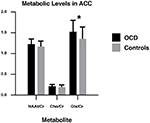
Figure 2. NAAt/Cr, Cho/Cr, and Glx/Cr concentrations in obsessive-compulsive disorder (OCD) patients and healthy controls in the ACC. NAAt, Full Due north-acetyl-aspartate; Cho, choline; Glx, glutamate–glutamine; Cr, creatine + phosphocreatine. ACC, inductive cingulate cortex. *p < 0.05.
Correlation Between H1-MRS Findings and Clinical Data
A correlational assay was fabricated to investigate if the college levels of Glx/Cr found in patients were related to symptom severity or disease duration, but no statistically meaning results emerged (p = 0.931 and r = 0.019, and p = 0.15 and r = 0.31, respectively; see Supplementary Material). Every bit our OCD sample was nether pharmacotherapy at the time of the scans, a medication score was created for each group of medication (i.e., SRIs and antipsychotics) co-ordinate to the equivalent dosage administrated. Then, a correlation analysis was performed betwixt the metabolic ratios and the scores for each patient on each group of medication. Although nosotros were unable to find whatsoever significant correlation between different metabolic ratios and the OCD patients' SRI (p = 0.088 and r = 0.373 for NAAt/Cr, p = 0.119 and r = 0.342 for Cho/Cr, and p = 0.17 and r = 0.303 for Glx/Cr) and antipsychotics' scores (p = 0.073 and r = −0.381 for NAAt/Cr, p = 0.106 and r = 0.346 for Cho/Cr, and p = 0.726 and r = 0.077 for Glx/Cr), 2 trends were particularly noticeable, i.e., a positive correlation between the NAAt/Cr and the SRI'south scores (p = 0.088 and r = 0.373) and a negative correlation between NAAt/Cr levels and antipsychotics' score (p = 0.073 and r = 0.381; Supplementary Textile). However, these findings did not survive statistical correction. Lack of relationships with medication use was confirmed by comparing the metabolic ratios in the ACC of OCD patients using SRI minus (SRI − ANP) vs. SRI plus antipsychotic (SRI + ANP; meet Supplementary Cloth).
Diffusion Tensor Imaging Findings
Voxelwise analysis showed no differences in FA and Medico between OCD patients and healthy volunteers. However, ROI analysis showed lower FA in the left CB (p = 0.034, Figure 3) of OCD patients compared to good for you controls. Values of MD did not differ significantly betwixt groups.
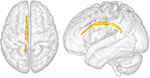
Figure iii. Comparing betwixt OCD patients and healthy controls in the left cingulate bundle (CB). Region of interest (ROI) analysis betwixt groups. Clusters of voxels significantly different (p < 0.05) are shown in red for fractional anisotropy (FA) in the white matter (WM). p = 0.034.
Improvidence Tensor Imaging Findings and Clinical Data
Significant correlations were found betwixt the severity of symptoms and WM integrity. We establish a meaning negative correlation betwixt Y-BOCS total score and FA value in left CB (p = 0.044 and r = 0.510), but information technology failed to survive the adjustments for depression and treatment score. We too constitute a significant negative correlation between Y-BOCS obsession subscore and FA value in right CB (p = 0.032 and r = 0.498) that also failed to survive the covariation assay. Further, we plant a significant negative correlation between Y-BOCS obsession subscore and FA value in left CB (r = 0.458; Figure 4). This correlation remained pregnant after depression (p = 0.039), antipsychotics (p = 0.010), and SRI scores (p = 0.014) were statistically controlled. Regarding the duration of the illness, nosotros found a significant negative correlation with FA values and CB (both left p = 0.033 and r = 0.494 and right p = 0.048 and r = 0.551) and positive correlations between Doctor value and correct CB (significant p = 0.005 and r = 0.498) and left CB (trend p = 0.057; Figure 5).
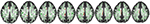
Figure 4. Negative correlation between Y-BOCS obsession score and FA in the left CB. Centric slices. Clusters of voxels significantly different (p < 0.05) are shown in ruddy for FA in the WM. p = 0.009.
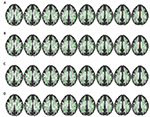
Figure five. Correlations between FA and mean diffusivity (MD) values and the duration of the affliction. Axial slices. Clusters of voxels significantly dissimilar (p < 0.05) are shown in blood-red for FA and in blue for Medico in the WM. (A,B) Negative correlation betwixt FA value and years of illness in right (p = 0.048) and left (p = 0.033) CB. (C,D) Positive correlation between MD value and years of illness in right CB (p = 0.005) and a trend in left CB (p = 0.057).
Correlation Between Structural and Metabolic Data
We investigated the association between Glx/Cr levels in ACC with FA values in the CB but failed to find any significant results (p = 0.794 and r = −0.041 for left CB; and p = 0.560 and r = 0.090 for right CB; see Supplementary Information).
Discussion
We performed a novel and simultaneous investigation of metabolic and structural alterations in OCD patients using 1H-MRS and DTI, respectively. Starting time, metabolic ratios in the ACC in 23 OCD patients and 21 healthy volunteers were compared. The findings revealed higher concentrations of Glx/Cr in OCD patients' ACC compared to healthy controls (p = 0.016). However, Glx/Cr did not correlate with the severity of the symptoms (YBOCS score; p = 0.931) or with the elapsing of the affliction (p = 0.15). Similarly, two previous studies reported significantly higher Glx levels in unmedicated OCD patients every bit compared to controls, one in the orbitofrontal cortex (Whiteside et al., 2006) and the other in the ACC (Gnanavel et al., 2014). Thus, 1H-MRS findings in the CB seem to be consistent with the hyperglutamatergic model of OCD, which describes high levels of glutamate in other parts of the CSTC system, such as the orbitofrontal and striatal regions (Rosenberg et al., 2000; Brennan et al., 2013). Indeed, in light of glutamate dysregulation in OCD, there is clinical evidence for the therapeutic utility of glutamate-modulating drugs as an augmentation or monotherapy in OCD patients. These drugs include memantine, anti-convulsant drugs, riluzole, and ketamine (Marinova et al., 2017). Among these, memantine appears to have greater potential (Sheshachala and Narayanaswamy, 2019).
We have also investigated the integrity of the WM in OCD patients compared to good for you controls, firstly by assessing FA and MD through whole-brain TBSS in all WM of OCD patients and controls, and and then by placing ROIs on CB (a disquisitional region of the CSTC loop) of the same enquiry subjects. Similarly to previous studies in children and adolescents (Jayarajan et al., 2012; Silk et al., 2013), our whole-brain analysis did non discover significant differences betwixt adult patients and controls in FA or Medico measurement. Even so, significantly lower FA values were observed in OCD patients' left CB as compared to good for you controls in the ROI analysis (p = 0.034). Accordingly, reductions of FA in the left anterior cingulate take been reported in both male and female (Lázaro et al., 2014) or just male OCD patients (Ha et al., 2009). Reduced FA values in patients with OCD may bespeak changes in myelination or disorganization of fibers within the packet. Regions that are interconnected by CBs include the prefrontal cortex, the parahippocampal areas, and the striatum (Lochner et al., 2012; Radua et al., 2014). These data advise microstructural abnormalities in CSTC loops encompassing ACC.
Importantly, we found a negative correlation between FA and severity of obsessions in the left CB (p = 0.009), suggesting that the more than severe the obsessive symptoms, the lower the integrity of this package. Although we could non perform a straight crusade-and-consequence analysis, this correlation could support the role of the CB (and its related circuits) in the neurobiology of OCD. Reinforcing the interest of this circuitry in OCD, we also found that the longer the duration of the disease, the lower the FA in CB (p = 0.048 for the right CB and p = 0.033 for the left CB), suggesting that bundle disorganization is either a consequence of or a risk factor for long-standing OCD. In the same line, disease duration also positively correlated with Dr. in right CB and, on a trend level, in left CB (p = 0.005 and p = 0.057, respectively). In addition, the previous written report of the lack of WM impairment in younger OCD samples (Jayarajan et al., 2012; Silk et al., 2013) may be consistent with the duration-related impairment of this circuitry in OCD.
Then, nosotros sought to explore whether CB integrity was related to regional neurochemistry. Nosotros hypothesized that abnormalities in WM integrity (i.e., reduced FA) would be negatively correlated with college levels of Glx in patients. More than specifically, we predicted that elevated levels of glutamate could pb to excitotoxicity that could influence the integrity of their axons or their connections. However, in contrast to our initial hypothesis, the Glx levels did not correlate with the FA in the CB. A possible reason for the absence of correlation between these parameters is that the increase in Glx may non have been sufficiently large to be neurotoxic.
In order to evaluate the influence of the medication on the metabolic concentrations of the ACC and WM integrity, a dose equivalence score was created for both SRIs and antipsychotics followed by a correlation analysis with the metabolic ratios and DTI values. The analysis showed no significant correlation between the scores and the imaging results. In addition, the sample of patients was separated into 2 groups: those who used SRIs and those who, also using SRIs, were also on antipsychotics. Metabolic ratios in the ACC between patient groups were compared, and no meaningful differences were found that could prove the influence of these substances in the metabolite'south ratios. That is, pharmacological treatment with antipsychotics did not seem to touch on the H1-MRS variables in our OCD patients, a finding that had already been reported in previous studies in OCD children and adolescents (Ortiz et al., 2015).
Our written report has some limitations. Kickoff, our OCD patients were nether active treatment. Although the inclusion of medicated OCD patients can be considered a major drawback of our study, our analyses took into account the relative dose of medications being used in an try to command the outcome of SRIs and antipsychotics. Second, possible patients' comorbidities were non addressed. Therefore, some could ascribe part of our findings to a higher severity of depressive symptoms in OCD patients every bit compared to healthy controls. Nevertheless, in contrast to our findings in this OCD cohort, meta-analysis of MRS studies in patients with depression did not show increased simply rather decreased glutamate levels in ACC (Luykx et al., 2012). Third, nosotros did not distinguish between glutamate and glutamine levels when using the Glx mensurate. Nevertheless, the fact that we used a 3.0-T machine, which has greater accuracy in the quantification of metabolites, has probably minimized the effects of this limitation (Paiva et al., 2013).
Finally, the fact that metabolic concentrations were corrected for Cr levels, instead of being absolutely quantified, could also be seen as a systematic limitation. Although the latter methodology is very widely applied and useful for clinical diagnosis (Jansen et al., 2006), metabolic concentrations corrected for Cr levels assume that there are no differences in the levels of Cr between patients and healthy volunteers, a premise that may not necessarily be truthful, since changes in Cr concentrations take already been reported in other psychiatric disorders such as schizophrenia and bipolar disorder (Ongür et al., 2009).
Conclusion
Thus, summing up, our findings reinforce the interest of CSTC and bundles that connect areas within the circuitry in pathophysiology of OCD. Further researches are needed with larger samples taking into account the dimensions of OCD to ameliorate understand how these changes correlate with the heterogeneous clinical/phenotypic presentations of OCD.
Ethics Statement
This written report was carried out in accord with the recommendations of the local ethics guidelines, with written informed consent from all subjects. All subjects gave written informed consent in accord with the Declaration of Helsinki. The protocol was approved by the ethics commission from D'Or Found for Research and Education.
Author Contributions
FT-One thousand, LF, and MY designed the study. IF, PV, JSA, and FF acquired the data, which MM, FF, and CS analyzed. JSA, IF, and FT-1000 wrote the commodity, which all authors reviewed and canonical for publication.
Funding
This work was supported past Conselho Nacional de Desenvolvimento Científico eastward Tecnológico (CNPq; LF, grant number 302526/2018-8), Fundação de Amparo à Pesquisa do Estado practise Rio de Janeiro (FAPERJ; LF, grant number CNE E-26/203.052/2017), also as by intramural grants from D'Or Found for Research and Education (IDOR). This written report was financed in office by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior–Brasil (CAPES)–Finance Code 001. MY has received funding from Monash University and Australian Authorities funding bodies such as the National Wellness and Medical Research Council (NHMRC; including Fellowship #APP1117188), the Australian Enquiry Quango (ARC), and the Department of Industry, Innovation and Science. He has too received philanthropic donations from the David Winston Turner Endowment Fund, as well as payment from law firms in relation to courtroom and/or expert witness reports. The funding sources had no part in study design, data assay, and event interpretation.
Disharmonize of Interest Statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed every bit a potential disharmonize of interest.
Acknowledgments
We are thankful to Débora Oliveira and all the technical team for their back up in unlike parts of the study and data acquisition. We also thank all volunteers for their participation in the study.
Supplementary Fabric
The Supplementary Material for this commodity tin be found online at: https://www.frontiersin.org/articles/10.3389/fnhum.2019.00186/full#supplementary-material
References
Admon, R., Bleich-Cohen, M., Weizmant, R., Poyurovsky, M., Faragian, S., and Hendler, T. (2012). Functional and structural neural indices of risk aversion in obsessive-compulsive disorder (OCD). Psychiatry Res. 203, 207–213. doi: ten.1016/j.pscychresns.2012.02.002
PubMed Abstract | CrossRef Full Text | Google Scholar
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders. Arlington, VA: American Psychiatric Publishing.
Google Scholar
Arnold, P. D., Macmaster, F. P., Hanna, G. Fifty., Richter, M. A., Sicard, T., Burroughs, E., et al. (2009). Glutamate system genes associated with ventral prefrontal and thalamic volume in pediatric obsessive-compulsive disorder. Brain Imaging Behav. three, 64–76. doi: 10.1007/s11682-008-9050-3
PubMed Abstruse | CrossRef Full Text | Google Scholar
Arun, P., Madhavarao, C. N., Moffett, J. R., Hamilton, 1000., Grunberg, N. E., Ariyannur, P. South., et al. (2010). Metabolic acetate therapy improves phenotype in the tremor rat model of Canavan disease. J. Inherit. Metab. Dis. 33, 195–210. doi: 10.1007/s10545-010-9100-z
PubMed Abstract | CrossRef Full Text | Google Scholar
Bhattacharyya, S., Khanna, Due south., Chakrabarty, K., Mahadevan, A., Christopher, R., and Shankar, Due south. K. (2009). Anti-encephalon autoantibodies and altered excitatory neurotransmitters in obsessive-compulsive disorder. Neuropsychopharmacology 34, 2489–2496. doi: 10.1038/npp.2009.77
PubMed Abstract | CrossRef Total Text | Google Scholar
Bora, E., Harrison, B. J., Fornito, A., Cocchi, L., Pujol, J., Fontenelle, L. F., et al. (2011). White affair microstructure in patients with obsessive-compulsive disorder. J. Psychiatry Neurosci. 36, 42–46. doi: x.1503/jpn.100082
PubMed Abstract | CrossRef Full Text | Google Scholar
Brennan, B. P., Rauch, S. 50., Jensen, J. Eastward., and Pope, H. Thou. Jr. (2013). A critical review of magnetic resonance spectroscopy studies of obsessive-compulsive disorder. Biol. Psychiatry 73, 24–31. doi: 10.1016/j.biopsych.2012.06.023
PubMed Abstract | CrossRef Full Text | Google Scholar
Carlsson, Yard. L. (2001). On the role of prefrontal cortex glutamate for the antithetical phenomenology of obsessive compulsive disorder and attending deficit hyperactivity disorder. Prog. Neuropsychopharmacol. Biol. Psychiatry 25, five–26. doi: 10.1016/s0278-5846(00)00146-9
PubMed Abstract | CrossRef Full Text | Google Scholar
Catheline, Thousand., Periot, O., Amirault, M., Braun, Yard., Dartigues, J. F., Auriacombe, S., et al. (2010). Distinctive alterations of the cingulum bundle during aging and Alzheimer's disease. Neurobiol. Aging 31, 1582–1592. doi: 10.1016/j.neurobiolaging.2008.08.012
PubMed Abstract | CrossRef Full Text | Google Scholar
Chakraborty, G., Mekala, P., Yahya, D., Wu, G., and Ledeen, R. Westward. (2001). Intraneuronal N-acetylaspartate supplies acetyl groups for myelin lipid synthesis: show for myelin-associated aspartoacylase. J. Neurochem. 78, 736–745. doi: 10.1046/j.1471-4159.2001.00456.x
PubMed Abstract | CrossRef Full Text | Google Scholar
Chamberlain, S. R., Blackwell, A. D., Fineberg, Due north. A., Robbins, T. W., and Sahakian, B. J. (2005). The neuropsychology of obsessive compulsive disorder: the importance of failures in cognitive and behavioural inhibition as candidate endophenotypic markers. Neurosci. Biobehav. Rev. 29, 399–419. doi: ten.1016/j.neubiorev.2004.11.006
PubMed Abstract | CrossRef Full Text | Google Scholar
Chiappelli, J., Hong, L. East., Wijtenburg, S. A., Du, X., Gaston, F., Kochunov, P., et al. (2015). Alterations in frontal white matter neurochemistry and microstructure in schizophrenia: implications for neuroinflammation. Transl. Psychiatry 5:e548. doi: 10.1038/tp.2015.43
PubMed Abstract | CrossRef Full Text | Google Scholar
Cunha, J. A. (2001). Manual da Versão em Português das Escalas Brook. São Paulo: Casa exercise Psicólogo.
Del-Ben, C. Thousand., Vilela, J. A., Crippa, J. A., Hallaka, J. E., Labate, C. Thousand., and Zuardi, A. W. (2001). Reliability of the structured clinical interview for DSM-IV—clinical version translated into Portuguese. Rev. Bras. Psiquiatr. 23, 156–159. doi: ten.1590/s1516-44462001000300008
CrossRef Full Text | Google Scholar
Fineberg, North. A., Stein, D. J., Premkumar, P., Carey, P., Sivakumaran, T., Vythilingum, B., et al. (2006). Adjunctive quetiapine for serotonin reuptake inhibitor-resistant obsessive-compulsive disorder: a meta-analysis of randomized controlled treatment trials. Int. Clin. Psychopharmacol. 21, 337–343. doi: ten.1097/01.yic.0000215083.57801.11
PubMed Abstract | CrossRef Full Text | Google Scholar
Fontenelle, L. F., Bramati, I. E., Moll, J., Mendlowicz, M. V., de Oliveira-Souza, R., and Tovar-Moll, F. (2011). White matter changes in OCD revealed by improvidence tensor imaging. CNS Spectr. 16, 101–109. doi: 10.1017/S1092852912000260
PubMed Abstract | CrossRef Full Text | Google Scholar
Garibotto, V., Scifo, P., Gorini, A., Alonso, C. R., Brambati, S., Bellodi, L., et al. (2010). Disorganization of anatomical connectivity in obsessive compulsive disorder: a multi-parameter diffusion tensor imaging report in a subpopulation of patients. Neurobiol. Dis. 37, 468–476. doi: 10.1016/j.nbd.2009.11.003
PubMed Abstract | CrossRef Total Text | Google Scholar
Gnanavel, S., Sharan, P., Khandelwal, S., Sharma, U., and Jagannathan, N. R. (2014). Neurochemicals measured by (1)H-MR spectroscopy: putative vulnerability biomarkers for obsessive compulsive disorder. MAGMA 27, 407–417. doi: 10.1007/s10334-013-0427-y
PubMed Abstract | CrossRef Full Text | Google Scholar
Goodman, W. 1000., Price, 50. H., Rasmussen, S. A., Mazure, C., Fleischmann, R. L., Hill, C. L., et al. (1989). The Yale-Brown obsessive compulsive scale I. Development, use and reliability. Arch. Gen. Psychiatry 46, 1006–1011. doi: 10.1001/archpsyc.1989.01810110048007
PubMed Abstract | CrossRef Total Text | Google Scholar
Govindaraju, Five., Young, K., and Maudsley, A. A. (2000). Proton NMR chemical shifts and coupling constants for brain metabolites. NMR Biomed. 13, 129–153. doi: 10.1002/1099-1492(200005)13:3<129::assistance-nbm619>3.3.co;2-m
PubMed Abstract | CrossRef Full Text | Google Scholar
Grados, 1000. A., Specht, M. W., Sung, H. M., and Fortune, D. (2013). Glutamate drugs and pharmacogenetics of OCD: a pathway-based exploratory approach. Expert Opin. Drug Discov. eight, 1515–1527. doi: ten.1517/17460441.2013.845553
PubMed Abstract | CrossRef Total Text | Google Scholar
Ha, T. H., Kang, D. H., Park, J. Southward., Jang, J. H., Jung, W. H., Choi, J. Due south., et al. (2009). White matter alterations in male patients with obsessive-compulsive disorder. Neuroreport 20, 735–739. doi: x.1097/WNR.0b013e32832ad3da
PubMed Abstract | CrossRef Full Text | Google Scholar
Jansen, J. F., Backes, W. H., Nicolay, K., and Kooi, M. Eastward. (2006). 1H MR spectroscopy of the encephalon: accented quantification of metabolites. Radiology 240, 318–332. doi: 10.1148/radiol.2402050314
PubMed Abstract | CrossRef Full Text | Google Scholar
Jayarajan, R. North., Venkatasubramanian, Grand., Viswanath, B., Janardhan Reddy, Y. C., Srinath, S., Vasudev, M. K., et al. (2012). White affair abnormalities in children and adolescents with obsessive-compulsive disorder: a diffusion tensor imaging written report. Depress Anxiety 29, 780–788. doi: 10.1002/da.21890
PubMed Abstruse | CrossRef Full Text | Google Scholar
Koch, K., Reeß, T., Rus, G., Zimmer, C., and Zaudig, M. (2014). Diffusion tensor imaging (DTI) studies in patients with obsessive-compulsive disorder (OCD): a review. J. Psychiatr. Res. 54, 26–35. doi: 10.1016/j.jpsychires.2014.03.006
PubMed Abstract | CrossRef Full Text | Google Scholar
Kohlrausch, F. B., Giori, I. Thou., Melo-Felippe, F. B., Vieira-Fonseca, T., Velarde, L. One thousand., de Salles Andrade, J. B., et al. (2016). Association of GRIN2B gene polymorphism and obsessive compulsive disorder and symptom dimensions: a airplane pilot study. Psychiatry Res. 243, 152–155. doi: x.1016/j.psychres.2016.06.027
PubMed Abstract | CrossRef Total Text | Google Scholar
Lázaro, 50., Calvo, A., Ortiz, A. Chiliad., Ortiz, A. East., Morer, A., Moreno, Due east., et al. (2014). Microstructural brain abnormalities and symptom dimensions in child and adolescent patients with obsessive-compulsive disorder: a diffusion tensor imaging report. Depress Anxiety 31, 1007–1017. doi: 10.1002/da.22330
PubMed Abstract | CrossRef Full Text | Google Scholar
Lochner, C., Fouche, J. P., du Plessis, S., Spottiswoode, B., Seedat, S., Fineberg, Due north., et al. (2012). Evidence for partial anisotropy and mean diffusivity white matter abnormalities in the internal capsule and cingulum in patients with obsessive-compulsive disorder. J. Psychiatry Neurosci. 37, 193–199. doi: 10.1503/jpn.110059
PubMed Abstract | CrossRef Full Text | Google Scholar
Luykx, J. J., Laban, K. G., van den Heuvel, Thou. P., Boks, M. P., Mandl, R. C., Kahn, R. S., et al. (2012). Region and country specific glutamate downregulation in major depressive disorder: a meta-analysis of (one)H-MRS findings. Neurosci. Biobehav. Rev. 36, 198–205. doi: ten.1016/j.neubiorev.2011.05.014
PubMed Abstract | CrossRef Full Text | Google Scholar
Madhavarao, C. N., Arun, P., Moffett, J. R., Szucs, S., Surendran, South., Matalon, R., et al. (2005). Lacking N-acetylaspartate catabolism reduces brain acetate levels and myelin lipid synthesis in Canavan'southward disease. Proc. Natl. Acad. Sci. U S A 102, 5221–5226. doi: 10.1073/pnas.0409184102
PubMed Abstract | CrossRef Full Text | Google Scholar
Marinova, Z., Chuang, D. Grand., and Fineberg, North. (2017). Glutamate-modulating drugs as a potential therapeutic strategy in obsessive-compulsive disorder. Curr. Neuropharmacol. 15, 977–995. doi: 10.2174/1570159x15666170320104237
PubMed Abstract | CrossRef Full Text | Google Scholar
McDonald, J. West., Althomsons, Southward. P., Hyrc, K. Fifty., Choi, D. W., and Goldberg, M. P. (1998). Oligodendrocytes from forebrain are highly vulnerable to AMPA/kainate receptor-mediated excitotoxicity. Nat. Med. 4, 291–297. doi: x.1038/nm0398-291
PubMed Abstract | CrossRef Full Text | Google Scholar
Meyer, J. H., Wilson, A. A., Sagrati, S., Hussey, D., Carella, A., Potter, West. Z., et al. (2004). Serotonin transporter occupancy of v selective serotonin reuptake inhibitors at different doses: an [11C]DASB positron emission tomography written report. Am. J. Psychiatry 161, 826–835. doi: 10.1176/appi.ajp.161.v.826
PubMed Abstract | CrossRef Full Text | Google Scholar
Modarresi, A., Sayyah, M., Razooghi, S., Eslami, Chiliad., Javadi, One thousand., and Kouti, L. (2018). Memantine augmentation improves symptoms in serotonin reuptake inhibitor-refractory obsessive-compulsive disorder: a randomized controlled trial. Pharmacopsychiatry 51, 263–269. doi: 10.1055/due south-0043-120268
PubMed Abstract | CrossRef Full Text | Google Scholar
Nakamae, T., Narumoto, J., Sakai, Y., Nishida, S., Yamada, K., Nishimura, T., et al. (2011). Diffusion tensor imaging and tract-based spatial statistics in obsessive-compulsive disorder. J. Psychiatr. Res. 45, 687–690. doi: 10.1016/j.jpsychires.2010.09.016
PubMed Abstract | CrossRef Full Text | Google Scholar
Ongür, D., Prescot, A. P., Jensen, J. E., Cohen, B. M., and Renshaw, P. F. (2009). Creatine abnormalities in schizophrenia and bipolar disorder. Psychiatry Res. 172, 44–48. doi: ten.1016/j.pscychresns.2008.06.002
PubMed Abstract | CrossRef Full Text | Google Scholar
Ortiz, A. E., Ortiz, A. M., Falcon, C., Morer, A., Plana, M. T., Bargalló, Northward., et al. (2015). 1H-MRS of the anterior cingulate cortex in childhood and adolescent obsessive-compulsive disorder: a case-command report. Eur. Neuropsychopharmacol. 25, threescore–68. doi: 10.1016/j.euroneuro.2014.11.007
PubMed Abstruse | CrossRef Full Text | Google Scholar
Paiva, F. F., Otaduy, M. C. G., de Oliveira-Souza, R., Moll, J., Bramati, I. E., Oliveira, Fifty., et al. (2013). Comparison of human encephalon metabolite levels using 1H MRS at ane.5T and 3.0T. Dement. Neuropsychol. 7, 216–220. doi: 10.1590/S1980-57642013DN70200013
PubMed Abstract | CrossRef Full Text | Google Scholar
Piras, F., Piras, F., Caltagirone, C., and Spalletta, One thousand. (2013). Brain circuitries of obsessive-compulsive disorder: a systematic review and meta-assay of tensor imaging studies. Neurosci. Biobehav. Rev. 37, 2856–2877. doi: 10.1016/j.neubiorev.2013.10.008
PubMed Abstruse | CrossRef Full Text | Google Scholar
Pittenger, C., Bloch, Yard. H., and Williams, M. (2011). Glutamate abnormalities in obsessive compulsive disorder: neurobiology, pathophysiology, and treatment. Pharmacol. Ther. 132, 314–332. doi: ten.1016/j.pharmthera.2011.09.006
PubMed Abstract | CrossRef Full Text | Google Scholar
Pittenger, C., Krystal, J. H., and Coric, V. (2006). Glutamate-modulating drugs as novel pharmacotherapeutic agents in the treatment of obsessive-compulsive disorder. NeuroRx iii, 69–81. doi: 10.1016/j.nurx.2005.12.006
PubMed Abstract | CrossRef Full Text | Google Scholar
Radua, J., Grau, Chiliad., van den Heuvel, O. A., Thiebaut de Schotten, M., Stein, D. J., Canales-Rodriguez, E. J., et al. (2014). Multimodal voxel-based meta-analysis of white thing abnormalities in obsessive-compulsive disorder. Neuropsychopharmacology 39, 1547–1557. doi: 10.1038/npp.2014.5
PubMed Abstract | CrossRef Full Text | Google Scholar
Rauch, South. L. (2003). Neuroimaging and neurocircuitry models pertaining to the neurosurgical treatment of psychiatric disorders. Neurosurg. Clin. Due north. Am. 14, 213–223. doi: 10.1016/s1042-3680(02)00114-6
PubMed Abstruse | CrossRef Full Text | Google Scholar
Reid, Yard. A., White, D. M., Kraguljac, N. V., and Lahti, A. C. (2016). A combined improvidence tensor imaging and magnetic resonance spectroscopy study of patients with schizophrenia. Schizophr. Res. 170, 341–350. doi: 10.1016/j.schres.2015.12.003
PubMed Abstruse | CrossRef Full Text | Google Scholar
Rodriguez, C. I., Kegeles, L. S., Levinson, A., Feng, T., Marcus, Southward. 1000., Vermes, D., et al. (2013). Randomized controlled crossover trial of ketamine in obsessive-compulsive disorder: proof-of-concept. Neuropsychopharmacology 38, 2475–2483. doi: 10.1038/npp.2013.150
PubMed Abstract | CrossRef Full Text | Google Scholar
Rosenberg, D. R., MacMaster, F. P., Keshavan, M. S., Fitzgerald, Thousand. D., Stewart, C. M., and Moore, G. J. (2000). Subtract in caudate glutamatergic concentrations in pediatric obsessive-compulsive disorder patients taking paroxetine. J. Am. Acad. Child Adolesc. Psychiatry 39, 1096–1103. doi: 10.1097/00004583-200009000-00008
PubMed Abstract | CrossRef Full Text | Google Scholar
Rowland, L. M., Spieker, E. A., Francis, A., Barker, P. B., Carpenter, W. T., and Buchanan, R. W. (2009). White matter alterations in deficit schizophrenia. Neuropsychopharmacology 34, 1514–1522. doi: 10.1038/npp.2008.207
PubMed Abstract | CrossRef Total Text | Google Scholar
Rueckert, D., Sonoda, L. I., Hayes, C., Hill, D. L., Leach, G. O., and Hawkes, D. J. (1999). Nonrigid registration using complimentary-form deformations: awarding to chest MR images. IEEE Trans. Med. Imaging 18, 712–721. doi: 10.1109/42.796284
PubMed Abstract | CrossRef Total Text | Google Scholar
Samuels, J., Wang, Y., Riddle, M. A., Greenberg, B. D., Fyer, A. J., McCracken, J. T., et al. (2011). Comprehensive family-based association study of the glutamate transporter gene SLC1A1 in obsessive-compulsive disorder. Am. J. Med. Genet. B Neuropsychiatr. Genet. 156B, 472–477. doi: 10.1002/ajmg.b.31184
PubMed Abstruse | CrossRef Full Text | Google Scholar
Saxena, S., Bota, R. G., and Brody, A. L. (2001). Encephalon-behavior relationships in obsessive-compulsive disorder. Semin. Clin. Neuropsychiatry 6, 82–101. doi: 10.1053/scnp.2001.21833
PubMed Abstract | CrossRef Full Text | Google Scholar
Shepherd, G. M. (2004). The Synaptic Arrangement of the Encephalon. 5th Edn. New York, NY: Oxford University Press.
Google Scholar
Sheshachala, Grand., and Narayanaswamy, J. C. (2019). Glutamatergic augmentation strategies in obsessive-compulsive disorder. Indian J. Psychiatry 61, S58–S65. doi: 10.4103/psychiatry.indianjpsychiatry_520_18
PubMed Abstruse | CrossRef Full Text | Google Scholar
Shugart, Y. Y., Wang, Y., Samuels, J. F., Grados, M. A., Greenberg, B. D., Knowles, J. A., et al. (2009). A family unit-based clan study of the glutamate transporter cistron SLC1A1 in obsessive-compulsive disorder in 378 families. Am. J. Med. Genet. B Neuropsychiatr. Genet. 150B, 886–892. doi: 10.1002/ajmg.b.30914
PubMed Abstruse | CrossRef Full Text | Google Scholar
Silk, T., Chen, J., Seal, M., and Vance, A. (2013). White matter abnormalities in pediatric obsessive-compulsive disorder. Psychiatry Res. 213, 154–160. doi: 10.1016/j.pscychresns.2013.04.003
PubMed Abstruse | CrossRef Full Text | Google Scholar
Simonyan, K., Tovar-Moll, F., Ostuni, J., Hallett, Thousand., Kalasinsky, Five. F., Lewin-Smith, Thou. R., et al. (2008). Focal white thing changes in spasmodic dysphonia: a combined diffusion tensor imaging and neuropathological study. Brain 131, 447–459. doi: 10.1093/brain/awm303
PubMed Abstract | CrossRef Total Text | Google Scholar
Simpson, H. B., Foa, E. B., Liebowitz, M. R., Huppert, J. D., Cahill, S., Maher, M. J., et al. (2013). Cognitive-behavioral therapy vs. risperidone for augmenting serotonin reuptake inhibitors in obsessive-compulsive disorder: a randomized clinical trial. JAMA Psychiatry 70, 1190–1199. doi: 10.1001/jamapsychiatry.2013.1932
PubMed Abstract | CrossRef Full Text | Google Scholar
Smith, S. M., Jenkinson, M., Johansen-Berg, H., Rueckert, D., Nichols, T. E., Mackay, C. E., et al. (2006). Tract-based spatial statistics: voxelwise assay of multi-subject improvidence data. Neuroimage 31, 1487–1505. doi: 10.1016/j.neuroimage.2006.02.024
PubMed Abstract | CrossRef Full Text | Google Scholar
Sookman, D., and Fineberg, N. A. (2015). Specialized psychological and pharmacological treatments for obsessive-compulsive disorder throughout the lifespan: a special serial by the Accreditation Task Force (ATF) of The Canadian Plant for Obsessive Compulsive Disorders (CIOCD, www.ciocd.ca). Psychiatry Res. 227, 74–77. doi: x.1016/j.psychres.2014.12.002
PubMed Abstract | CrossRef Total Text | Google Scholar
Steel, R. M., Bastin, M. E., McConnell, Due south., Marshall, I., Cunningham-Owens, D. G., Lawrie, Southward. One thousand., et al. (2001). Diffusion tensor imaging (DTI) and proton magnetic resonance spectroscopy (1H MRS) in schizophrenic subjects and normal controls. Psychiatry Res. 106, 161–170. doi: 10.1016/s0925-4927(01)00080-4
PubMed Abstract | CrossRef Full Text | Google Scholar
Lord's day, Z., Wang, F., Cui, 50., Breeze, J., Du, X., Wang, X., et al. (2003). Aberrant inductive cingulum in patients with schizophrenia: a diffusion tensor imaging study. Neuroreport 14, 1833–1836. doi: 10.1097/01.wnr.0000094529.75712.48
PubMed Abstract | CrossRef Full Text | Google Scholar
Szeszko, P. R., Ardekani, B. A., Ashtari, M., Malhotra, A. One thousand., Robinson, D. Grand., Bilder, R. Grand., et al. (2005). White matter abnormalities in obsessive-compulsive disorder: a diffusion tensor imaging study. Arch. Gen. Psychiatry 62, 782–790. doi: 10.1001/archpsyc.62.7.782
PubMed Abstract | CrossRef Full Text | Google Scholar
Tang, C. Y., Friedman, J., Shungu, D., Chang, 50., Ernst, T., Stewart, D., et al. (2007). Correlations between Diffusion Tensor Imaging (DTI) and Magnetic Resonance Spectroscopy (1H MRS) in schizophrenic patients and normal controls. BMC Psychiatry 7:25. doi: ten.1186/1471-244x-seven-25
PubMed Abstract | CrossRef Full Text | Google Scholar
Wang, R., Fan, Q., Zhang, Z., Chen, Y., Tong, S., and Li, Y. (2017). White matter integrity correlates with choline level in dorsal anterior cingulate cortex of obsessive-compulsive disorder patients: a combined DTI-MRS report. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2017, 3521–3524. doi: 10.1109/embc.2017.8037616
PubMed Abstract | CrossRef Full Text | Google Scholar
Wang, R., Fan, Q., Zhang, Z., Chen, Y., Zhu, Y., and Li, Y. (2018). Anterior thalamic radiation structural and metabolic changes in obsessive-compulsive disorder: a combined DTI-MRS study. Psychiatry Res. Neuroimaging 277, 39–44. doi: 10.1016/j.pscychresns.2018.05.004
PubMed Abstract | CrossRef Total Text | Google Scholar
Wang, J., Leone, P., Wu, Thousand., Francis, J. Southward., Li, H., Jain, Yard. R., et al. (2009). Myelin lipid abnormalities in the aspartoacylase-deficient tremor rat. Neurochem. Res. 34, 138–148. doi: ten.1007/s11064-008-9726-5
PubMed Abstract | CrossRef Full Text | Google Scholar
Whiteside, S. P., Port, J. D., Deacon, B. J., and Abramowitz, J. Southward. (2006). A magnetic resonance spectroscopy investigation of obsessive-compulsive disorder and anxiety. Psychiatry Res. 146, 137–147. doi: 10.1016/j.pscychresns.2005.12.006
PubMed Abstract | CrossRef Total Text | Google Scholar
Wijtenburg, S. A., McGuire, Southward. A., Rowland, L. M., Sherman, P. M., Lancaster, J. L., Tate, D. F., et al. (2013). Relationship between fractional anisotropy of cerebral white matter and metabolite concentrations measured using (i)H magnetic resonance spectroscopy in healthy adults. Neuroimage 66, 161–168. doi: 10.1016/j.neuroimage.2012.ten.014
PubMed Abstract | CrossRef Total Text | Google Scholar
Yücel, M., Wood, S. J., Wellard, R. Yard., Harrison, B. J., Fornito, A., Pujol, J., et al. (2008). Anterior cingulate glutamate-glutamine levels predict symptom severity in women with obsessive-compulsive disorder. Aust. Northward. Z. J. Psychiatry 42, 467–477. doi: x.1080/00048670802050546
PubMed Abstract | CrossRef Total Text | Google Scholar
Source: https://www.frontiersin.org/articles/10.3389/fnhum.2019.00186/full
0 Response to "what type of brain scan is needed to identify ocd"
Post a Comment